Why iCOPE?

Patients with cancer are best served by interdisciplinary care teams focused on their physical, psychosocial, and spiritual needs. Yet today’s clinicians are trained largely in academic silos and are ill-prepared and inexperienced in interdisciplinary care. The Institute of Medicine has called for health professionals to be educated in an interdisciplinary manner to prepare them for real world team environments. Palliative care is now recommended for all cancer patients from the time of diagnosis and is interdisciplinary by its very nature. iCOPE is designed to fill the gap in interprofessional palliative education and improve the care of patients with cancer.
Mandates for Interprofessional Education in Palliative Care
The need for interprofessional education in the healthcare professions was first formally recognized in the early 1970’s as a means to improve quality of care, safety and patient outcomes. Since then numerous reports from organizations such as the Institute of Medicine, the World Health Organization and the Macy Foundation have concluded that students of the various healthcare specialties need to learn to practice in teams, collaborate and communicate effectively and deliver patient-centered, holistic healthcare. Interprofessional education is necessary to prepare students to practice together and deliver team-based care when they enter the healthcare workforce.
Palliative care is by its very nature interprofessional care. Definitions of palliative care recognize that it is care provided by a team of professionals. The Clinical Practice Guidelines for Quality Palliative Care highlight the following domains. In domain 1: Structure and Processes of Care, Guideline 1.3 states “An interdisciplinary team (IDT) provides services to the patient and family consistent with the care plan.” (p.15). This team consists of chaplains, nurses, physicians, social workers and other therapeutic disciplines who provide care to palliative care patients.
The team approach insures holistic care which addresses not only the medical needs of the patient, but also the psychosocial and spiritual needs of the patient and family. In order to practice palliative care, it is essential that clinicians learn not only the unique knowledge and skills pertinent to their practice specialty but also develop the communication and collaboration skills necessary for effective teamwork.
The National Consensus Project for Quality Palliative Care. (2013). Clinical Practice Guidelines for Quality Palliative Care.
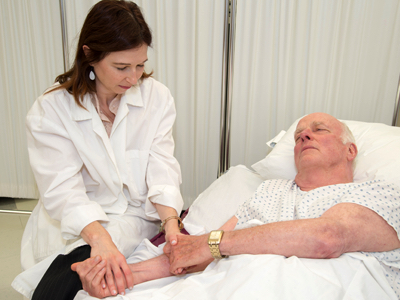
Dying in America
In September, 2014, the Institute of Medicine released the report, Dying in America: Improving Quality and Honoring Individual Preferences Near the End of Life. This report recommends that “educational institutions, professional societies, accrediting organizations, certifying bodies, health care delivery organizations and medical centers take measures to both increase the number of palliative care specialists and expand the knowledge base for all clinicians.” (IOM Report Brief, 2014) Furthermore, the recommendations call for all clinicians caring for people with advanced illness to become competent in communication and inter-professional collaboration – skills that are best taught through inter-professional education.
For more information see:
Committee on Approaching Death (2014), Dying in America: Improving Quality and Honoring Individual Preferences Near the End of Life. Washington, D.C.: Institute of Medicine.

